Bryan Cotton and his colleagues in the simulation lab don’t see patients, but they have indirectly saved the lives of countless people throughout the Dallas-Fort Worth area.
The Texas Health Harris Methodist Hospital Fort Worth simulation lab provides a realistic setting for all facets of health care education. Clients include paramedics, medical and nursing residents, chaplains and even high school students interested in health care.
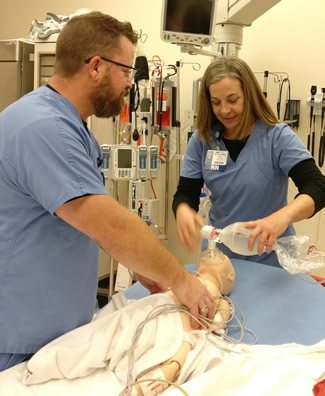
“We’re kind of the set designers,” said Cotton, a former firefighter and emergency medical technician. “We have different rooms reflecting different environments, so it’s like a set that revolves and changes. We make whatever it needs to be for any given scenario, no matter who we’re helping.”
Cotton and program manager Audra Lewis, Ph.D., R.N., CHSE, say the work involves a lot of collaboration and research.
“We’re not the content experts,” Lewis said. “We talk to the experts to get their ideas and understand their needs, then come up with a concept and present it to them to make sure it’s realistic.”
Some scenarios are easy to set up, but others require more work than others. They recently set up a simulation for Texas Health Cleburne when the hospital added an interventional radiology service line.
“We did a lot of research and looked at a lot of publications,” Lewis said. “We even went one day to watch some cases, so we could get a conceptual idea of what it should look like, feel like, sound like, even smell like. Then we came back here and re-created it, so the learners are immersed in the environment.”
Lifesaving lesson
Cotton and his colleagues rarely see the results of their work, but Meesha Crocker, a paramedic with MedStar Mobile Healthcare, recently contacted him to say that one course had helped her save a life just two weeks later.
Crocker had come to the lab for training and mentioned to Cotton that she had never performed a cricothyrotomy, a procedure in which a tube is placed through an incision in the cricothyroid membrane of the throat to establish an airway.
“So they gave me a scenario with a ‘patient,’” Crocker said. “The only clue I had was some paperwork they’d left saying he had started a new prescription, lisonopril for high blood pressure, which can cause angioedema.
“I went through the entire airway protocol, and I got to do a ‘cric’ on the dummy.”
Two weeks later, Crocker was called out to a home in Fort Worth. When she and her partner arrived, firefighters brought over the man, who was talking and walking on his own. The man said he had no allergies and wasn’t taking any medication, and his vital signs were close to normal.
“But you could see that his tongue was swollen,” she said. “I asked him specifically if he had high blood pressure or was taking lisinopril, and he said no. I thought it was an allergic reaction, but epinephrine and Benadryl weren’t helping.
“I thought if it walks like a duck, it probably is. I was able to inform my partner about what was going on, and we had all the airway equipment out before he needed it.”
Meanwhile, firefighters were talking to the man’s family in the house. When they came out with his paperwork, the forms said he was taking lisinopril.
“When I saw that, I told my partner, ‘It’s angioedema. He’s having a reaction to the ace inhibitor,’” Crocker said. “We both looked at him, and even though he had been stable and talking to us seconds before, that was his last breath.”
The “cric” needle wouldn’t puncture through the swelling, so Crocker knew she needed to do a surgical cricothyrotomy. Because the equipment was already out, they were able to secure the tube and stabilize the patient within six minutes.
“It happened so fast,” Crocker said. “If we hadn’t been prepared because of the scenario I ran in the sim lab — and because I was able to make mistakes in a safe environment and learn from them — we wouldn’t have been able to act so quickly.
“I texted Bryan afterward and said, ‘You saved a life tonight.’”
Award-winning innovation
Cotton and the sim lab’s impact reaches even farther, though. He recently received a Simulation Champion Award from SimGHOSTS, an international organization dedicated to supporting individuals and institutions operating medical simulation technology and spaces, for his creativity and altruism.
“Human simulators are a lot more sophisticated than Resusci Annie from the ‘70s,” Cotton said. “But there’s also a need to make things that don’t exist, and we need to get medical supplies without spending a lot.”
To keep costs down, Cotton collects expired medical supplies from throughout the system and repurposes objects to build new simulators.
“I refer to him as the simulation ambassador, because you can walk through the hospital with Bryan and he knows somebody around every corner,” Lewis said. “People even come here and bring their expired supplies.”
Cotton started working on simulations while teaching CPR and advanced cardiac life support in Dallas.
“I inherited all these old simulators that didn’t work; no one even knew how to turn them on,” said Cotton, who has been taking things apart and putting them back together since childhood. “I took parts from one to make another one work. Through all that, I learned simulation and got to know the sales reps.”
When he heard that Texas Health Fort Worth was opening a sim lab, he jumped at the opportunity.
“I wanted to serve the community,” he said. “We don’t just serve Texas Health Fort Worth. We serve all of Texas Health and all of the community, even our competitors.”
Lewis said one of Cotton’s recent inventions is one reason he received the award. He adapted a simulator that produces EKG rhythms to have multiple outputs.
“The simulator only has one output, but in some environments, you need multiple outputs,” he explained. “I put several together to get three outputs out of one device. So, for example, it allows you to look at the anesthesia card, the bedside monitor and the circulating cameras at the same time.
“I made it so you can almost just go to Hobby Lobby and make one. It uses supplies that everyone has and existing technology. It costs about 18 cents.”
Personalized training
The lab, with just two full-time and two part-time employees, stays busy, seeing about 150 learners a month. It has a lifelong fan in Crocker.
“People need to go to the sim lab on a regular basis,” she said. “It’s such an amazing program. Bryan made a point of telling me to let him know if there’s anything I need or want to work on.”
When she asked about pediatric intubation during her first visit, he jumped into action.
“He said, ‘OK, let’s do it,’” she recalled. “He took the whole class and had us intubate pediatric dummies of all sizes. Those cases don’t happen very often, but I don’t want those to be my learning experiences. I want those to be my treating experiences.”
Lewis said that’s typical.
“Bryan is very good at doing things on the fly,” she said. “And he makes it look easy.”
Related News
About Texas Health Resources
Texas Health Resources is a faith-based, nonprofit health system that cares for more patients in North Texas than any other provider. With a service area that consists of 16 counties and more than 8 million people, the system is committed to providing quality, coordinated care through its Texas Health Physicians Group and 29 hospital locations under the banners of Texas Health Presbyterian, Texas Health Arlington Memorial, Texas Health Harris Methodist and Texas Health Huguley. Texas Health access points and services, ranging from acute-care hospitals and trauma centers to outpatient facilities and home health and preventive services, provide the full continuum of care for all stages of life. The system has more than 4,400 licensed hospital beds, 6,400 physicians with active staff privileges and nearly 29,000 employees. For more information about Texas Health, call 1-877-THR-WELL, or visit www.TexasHealth.org.
