Cancers Screenings Are Not A Luxury
 When Ariana noticed a growing lump and persistent pain in her right breast, the uninsured Arlington mother turned to Texas Health’s Wellness for Life® Mobile Health Program. A friend had told her about the mobile units that bring screening mammograms, pap smears, and other preventive services directly into communities at no cost thanks to donor support. Ariana’s visit quickly led to a referral for diagnostic testing at the Kupferle Breast Center, where she learned she had Stage 3 triple‑negative breast cancer.
When Ariana noticed a growing lump and persistent pain in her right breast, the uninsured Arlington mother turned to Texas Health’s Wellness for Life® Mobile Health Program. A friend had told her about the mobile units that bring screening mammograms, pap smears, and other preventive services directly into communities at no cost thanks to donor support. Ariana’s visit quickly led to a referral for diagnostic testing at the Kupferle Breast Center, where she learned she had Stage 3 triple‑negative breast cancer.
For Ariana, that mobile health visit was life‑changing. “The mobile clinic was the start of it all,” she said. “If I had never gone there, I would have never realized I had breast cancer.” By reducing financial, transportation, and access barriers, the mobile health team ensures individuals who might otherwise delay care can get the critical screenings they need.
Today, Ariana is in treatment and shares her story to encourage others to seek preventive care. “I hope people find the courage to get checked,” Ariana said. “I’m just grateful it wasn’t too late for me. The faster you catch it, the better.”
They Never Stopped Fighting For Her
 At just 24 weeks pregnant, Annie faced a terrifying diagnosis: severe preeclampsia, placental abruption, and a baby with intrauterine growth restriction. Her local physicians told her she had two choices — provide comfort care or transfer to Texas Health Harris Methodist Fort Worth Hospital for a “trial of life.”
At just 24 weeks pregnant, Annie faced a terrifying diagnosis: severe preeclampsia, placental abruption, and a baby with intrauterine growth restriction. Her local physicians told her she had two choices — provide comfort care or transfer to Texas Health Harris Methodist Fort Worth Hospital for a “trial of life.”
Within hours, Annie was flown by helicopter to Texas Health Fort Worth, where an emergency C-section delivered baby Nora at only 13.1 ounces, roughly the size of a soda can. She was immediately placed in the hospital’s Level IV Neonatal Intensive Care Unit, equipped with advanced respiratory support and other technology necessary to save her life.
Over the next several months, Nora required highly specialized care, from delicate procedures to repair a heart defect to round‑the‑clock monitoring on state‑of‑the‑art equipment designed for micro-preemies. Her parents often describe the experience of holding their daughter, surrounded by wires and monitors, as both terrifying and miraculous. Thanks to advancements in neonatal medicine and the hospital’s continually upgraded NICU environment, Nora defied the odds.
Eight months after her birth, Nora came home weighing a healthy 10 pounds, a thriving reminder of what modern neonatal care makes possible. Parents Annie and Owen credit the skill of their care team and the life‑saving equipment. Their gratitude now fills their home, including a photo wall with the phrase: “I still remember the days I prayed for the things I have now.” Annie says it best: “I can’t thank them enough for believing in her. What they do is amazing.”
From Caregiver to Patient
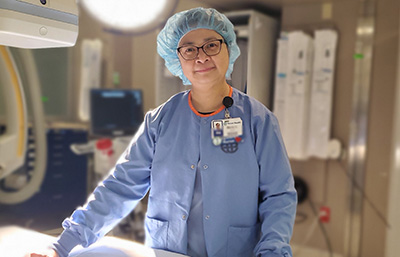 Marie, a cardiac electrophysiology specialist and 20‑year nurse, never imagined she would become the patient. But when a sudden tear in her mitral valve triggered acute heart failure, she found herself fighting for her life at Texas Health Presbyterian Hospital Dallas.
Marie, a cardiac electrophysiology specialist and 20‑year nurse, never imagined she would become the patient. But when a sudden tear in her mitral valve triggered acute heart failure, she found herself fighting for her life at Texas Health Presbyterian Hospital Dallas.
Over 22 days, Marie underwent an emergency valve replacement, relied on a mechanical heart pump — one of the smallest in the world — and received lifesaving Extracorporeal Membrane Oxygenation (ECMO) therapy to support her heart and lungs. She credits the rapid, coordinated care of her colleagues, and the advanced technology available at Texas Health with giving her a second chance at life.
Marie’s condition was so severe that multiple teams, from heart failure specialists to cardiothoracic surgeons, worked around the clock to uncover the cause of her rapid deterioration. Both the ECMO system and the mechanical pump sustained her while her care team discovered the root issue: critically low cortisol levels. Once treated, Marie began to stabilize. She remembers waking up shocked to learn she had been unconscious for more than a week and deeply moved by the compassion shown to her family.
Four months after surgery, Marie returned to work with a renewed sense of gratitude and purpose. Today, she shares her story with heart patients to reassure them that healing is possible, because she has lived it herself. Her experience reflects the power of exceptional clinical expertise, advanced equipment, and the culture at Texas Health. “It might seem bad right now,” she tells patients, “but it really can get better.”
Care That Feels Like Home
 When 55‑year‑old Yon collapsed from a heart attack and cardiac arrest while dining in North Texas, he had no idea how close he came to losing his life. Restaurant employees called 911, and paramedics quickly revived him with CPR and defibrillation before transporting him to Texas Health Presbyterian Hospital Plano. There, Yon received rapid, high‑quality cardiac care including emergency catheterization, a stent placement and intensive support in the ICU — care he credits with giving him a second chance at life.
When 55‑year‑old Yon collapsed from a heart attack and cardiac arrest while dining in North Texas, he had no idea how close he came to losing his life. Restaurant employees called 911, and paramedics quickly revived him with CPR and defibrillation before transporting him to Texas Health Presbyterian Hospital Plano. There, Yon received rapid, high‑quality cardiac care including emergency catheterization, a stent placement and intensive support in the ICU — care he credits with giving him a second chance at life.
His recovery was challenging. After surviving cardiac arrest, Yon developed severe pneumonia and spent 19 days on a ventilator. But the coordinated work of cardiologists, critical care teams, and respiratory therapists helped him steadily regain strength. After 32 days in the hospital, Yon returned home to North Carolina profoundly grateful and eager to reunite with the team that saved him. “I had a heart attack, I went into cardiac arrest, I developed pneumonia, but I still survived,” he said. “Texas Health Plano provided first‑class service.”
Months later, King flew more than 1,000 miles back to Texas to thank his caregivers in person. He says their rapid action, compassion, and expertise made all the difference. “I’m eternally grateful,” he shared. “Because of their actions, I can share my testimony and help others for the rest of my life.”
