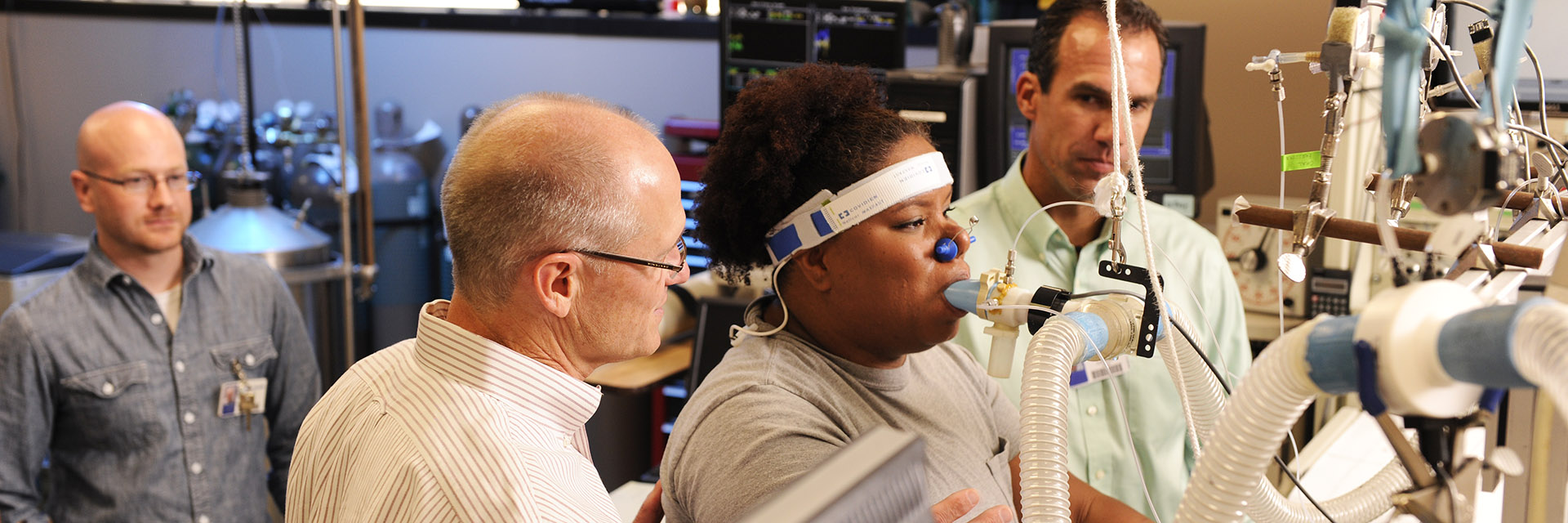
Pulmonary Physiology Laboratory
The global focus of the Pulmonary Physiology Laboratory is the study of pulmonary exercise physiology, particularly as it pertains to pulmonary disease, normal aging, obesity, ventilatory control during exercise, applied respiratory physiology, and clinical cardiopulmonary exercise testing. The Pulmonary Physiology Laboratory consists of three separate investigative laboratories: the pulmonary function laboratory, the cardiopulmonary exercise physiology laboratory, and the body composition laboratory including DEXA imaging for the determination of percent body fat, lean body mass, bone content, visceral fat, overall fat distribution, and their effects on breathing.
Currently, the Pulmonary Physiology Laboratory research focuses on investigating the respiratory effects of obesity in children, which is an extension of prior work on the mechanisms of exertional dyspnea in adults with obesity. The latest project investigates the mechanisms of dyspnea on exertion and exercise intolerance in in patients with heart failure with preserved ejection fraction (HFpEF) and the impact of obesity. Also, laboratory investigators have recently initiated research into the mechanisms of exercise intolerance and breathlessness in older adults with obesity.
Interests
Respiratory Effects of Obesity in Children
Over 19% of children 6-11 years old are classified as obese. We have found numerous obesity-related respiratory effects that could influence exercise tolerance and breathlessness in adults. However, it is unclear whether the obesity-related respiratory effects in adults can be extended to children. It is possible that respiratory effects could reduce exercise tolerance, provoke dyspnea on exertion, or contribute to respiratory symptoms. These symptoms could be misdiagnosed as asthma in children with obesity. Obesity-related respiratory symptoms are reported to be wrongly labeled ‘asthma’ in over 50% of patient cases placing children with obesity at risk of unnecessary treatment and potentially a reluctance to exercise, which is counterproductive to weight loss.
Pulmonary Mechanisms of Dyspnea in HFpEF: Impact of Obesity (Project 4 of a program project titled: Mechanisms of Exercise Intolerance in Heart Failure with Preserved Ejection Fraction: Precision Therapy Based on Patient Specific Pathophysiology)
Dyspnea on exertion and exercise intolerance are hallmark symptoms of heart failure with preserved ejection fraction (HFpEF). The mechanisms of these two symptoms are unknown in patients with HFpEF. Potential mechanisms are numerous and multifactorial, including breathing limitations (underlying lung dysfunction), exercise ventilatory limitations (reduced ventilatory reserves, expiratory flow limitation), central cardiovascular limitations (blunted cardiac output, heart stiffness), increased pulmonary capillary wedge pressure (PCW), peripheral vascular/muscle limitations (oxygen uptake, oxidative metabolism, & blood flow), autonomic control alterations (altered neural or vascular control), and lastly obesity (obesity related reduced lung function, increased work of breathing, etc.). Indeed, the effect of obesity in patients with HFpEF is underappreciated, in contrast to conventional thinking, which assumes that increased PCW alone is responsible for dyspnea on exertion (DOE) and exercise intolerance in patients with HFpEF. However, many of the changes noted in patients with HFpEF are common alterations related to obesity. However, it is unclear whether obesity amplifies HFpEF-related breathing limitations or is a sole contributor to DOE and/or exercise intolerance, but obesity is likely an under recognized but significant contributor to DOE in patients with HFpEF.
Mechanisms of Dyspnea on Exertion (DOE) in adults with Obesity
Our studies have shown that one third of otherwise healthy younger adults with obesity suffer from DOE. Although adults with obesity and DOE are generally considered to be deconditioned, our findings continue to challenge this misconception. Additionally, we have shown that excess fat on the chest wall exerts an unfavorable mechanical burden on the respiratory system, particularly during exercise, potentially contributing to DOE. Past studies have also shown that modest weight loss (WL) significantly reduces DOE in women with obesity, and likewise, endurance exercise training (ET) in women with obesity also reduces DOE. Overall, these studies are the first to show that WL and/or ET are effective treatments for DOE in adults with obesity; however, the mechanisms by which WL and ET decrease DOE remain unclear.
Respiratory Effects of Obesity in the Aged
Dr. Babb has recently initiated research studies investigating the mechanisms of exercise intolerance and breathlessness in older adults with obesity. Over 40% of older adults (60+ yr) are obese and 30% are overweight. While regular exercise is an important component in the prevention and treatment of obesity, many older adults with obesity are unable or unwilling to exercise due to exercise intolerance and/or dyspnea on exertion (DOE). We have identified numerous obesity-related effects that could influence exercise tolerance and DOE in younger obese adults including decreased pulmonary function, altered respiratory mechanics, increased work of breathing, and increased metabolic demands of exercise10,94. We have also identified many age-related ventilatory constraints in older adults without obesity. However, it is unclear whether these obesity-related and aging-related effects are exaggerated in older adults with obesity and whether they reduce exercise tolerance, provoke DOE, or contribute to respiratory symptoms. Respiratory symptoms in older adults are often wrongly diagnosed as exercise deconditioning and/or cardiopulmonary disease, placing older adults with obesity at risk of costly clinical testing, unnecessary treatment, and potentially a reluctance to exercise, which is counterproductive to weight loss and the preservation of functional capacity, thus further diminishing their quality of life. The effects of obesity are underappreciated and have not been carefully examined in older adults, especially those with “ respiratory symptoms.”
Current Projects
- Respiratory Effects of Obesity in Children
- Pulmonary Mechanisms of Dyspnea in HFpEF: The Impact of Obesity
- Effects of Obesity in the Aged
Current Research Opportunities
View our current Pulmonary Physiology research opportunities for:
- Breathing Limitations in Children with High Weight – Ages 8-12
- The Effects of Obesity in the Aged- Ages 65-75
- Short Term Modulation of the Exercise Ventilatory Response in Patients with Obesity Hypoventilation Syndrome
-
Principal Investigator
-
Postdoctoral Fellows / Residents
-
Staff
-
Weight loss reduces dyspnea on exertion in obese women
-
Aerobic exercise training without weight loss reduces dyspnea on exertion in obese women
-
Effect of weight loss on operational lung volumes and oxygen cost of breathing in obese women
-
Verification of Maximal Oxygen Uptake in Obese and Nonobese Children
-
Dyspnea on exertion provokes unpleasantness and negative emotions in women with obesity
-
Weight loss reduces dyspnea on exertion and unpleasantness of dyspnea in obese men
-
Quantification of Cardiorespiratory Fitness in Children with Obesity
-
Multidimensional aspects of dyspnea in obese patients referred for cardiopulmonary exercise testing
-
Reduced Physical Activity Levels in Children after a First Episode of Acute Venous Thromboembolism
-
External dead space explains sex-differences in the ventilatory response
-
Effects of obesity on the oxygen cost of breathing in children
-
Inhaled albuterol increases estimated ventilatory capacity in nonasthmatic children
-
Repeatability of dyspnea measurements during exercise in women with obesity
-
Estimating exercise PaCO2 in patients with heart failure with preserved ejection fraction
-
Physiological dead space during exercise in patients with heart failure with preserved ejection fraction