-
Vaginal Birth and Inductions
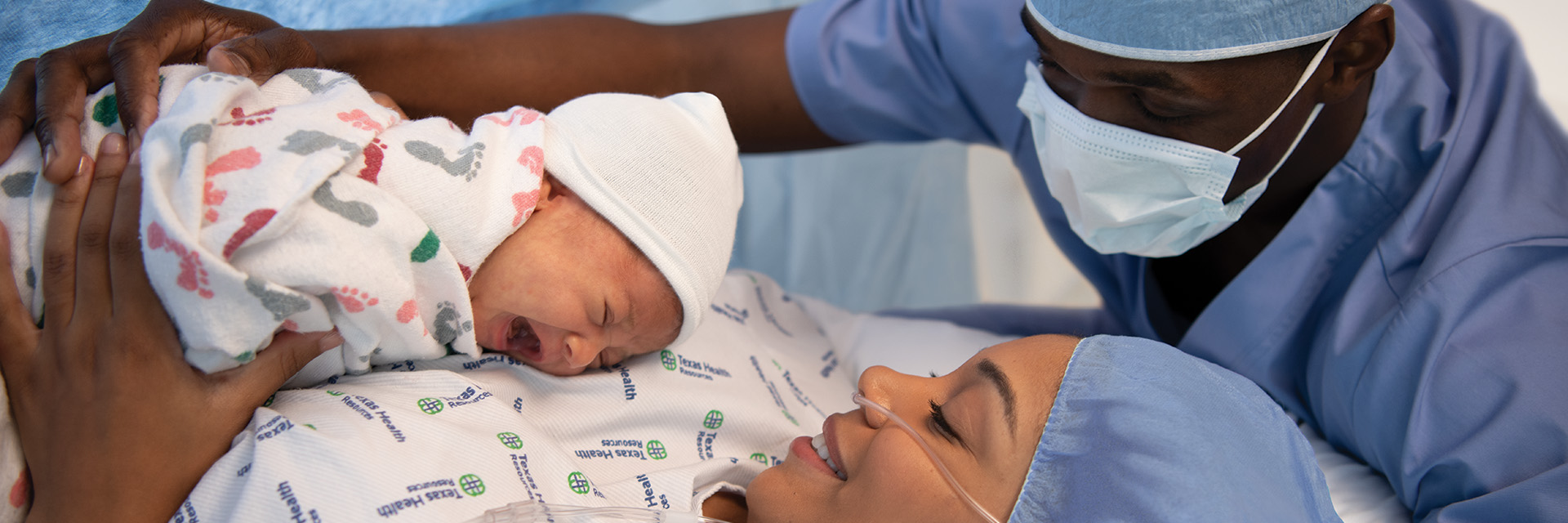
A vaginal birth is a reasonable goal for the majority of women. During a vaginal birth, a woman’s cervix dilates and contractions slowly increase in frequency. The contractions will become stronger as your body prepares to move the baby. Your provider will assist you in determining when to push and help the baby progress through the birth canal. Once the baby is born, the umbilical cord will be cut and baby will be handed to you for skin-to-skin contact. You may still experience some contractions as you gently deliver the placenta.
Being Induced
If you have a medical issue, you may have your labor induced. This means that your healthcare provider helps your uterus to start having contractions. To help start labor, your healthcare provider may break your water. Your body makes a hormone called oxytocin that makes the uterus contract. If you are not having contractions, your healthcare provider may give you a medicine that can start contractions or speed up labor.
-
Cesarean Birth
In a cesarean birth, the baby will come out through an incision in your belly. It is a major surgery. Cesarean births typically, take less than one hour. Your partner may be able to join you in the room. You may not plan to have a cesarean birth, but it may be the best thing for you and your baby.
Reasons for a Cesarean Birth
The following situations may make a vaginal birth risky for the baby:
- The baby's head is too large to pass through mother's pelvis
- The baby is positioned buttocks-first (breech)
- Medical conditions of the mother, such as hypertension, preeclampsia or eclampsia
- Premature labor
- Multiple babies
- Problems with the cervix, birth canal, umbilical cord or placenta
- A labor that stalls or progresses very slowly
- The fetal heartbeat slows, speeds up or becomes irregular during labor.
If the Cesarean is Planned
Typically, if you are having a scheduled induction or cesarean, you will be asked not to eat at least eight hours before the procedure or the procedure may be rescheduled. You will be prepared approximately two hours prior to the procedure. You'll receive a general or regional anesthetic (such as a spinal or an epidural) that numbs the lower half of your body but leaves you awake and alert.
During the surgery, your provider may take up to 10 minutes to deliver your baby and then placenta. Then your provider will close the incisions in your uterus and belly, which in total typically takes about an hour.
If an Emergency Cesarean is Needed
If an emergency cesarean is needed, your doctor may use general anesthesia, which takes effect almost immediately and renders you unconscious. In an emergency cesarean, it may only take two minutes for your baby to be born.
Gentle Cesareans
For those that need to have a cesarean birth, several of the Texas Health hospitals offer a type of cesarean that aims to create a birth experience similar to a vaginal delivery, called a gentle cesarean. During the surgery, the blue drape that is placed at the mom’s chest, which obstructs her view of the doctor and the delivery, can be replaced with a clear drape or a drape with a window. With the clear drape in place, the mother and support person can watch the baby being born, similar to seeing the birth of a baby during a vaginal delivery.
Please be aware that this option is not available at all the hospitals. If you are interested in this type of experience, please discuss it with your doctor.
Cesarean Birth Class
Texas Health offers a class to help families prepare for cesarean births.
-
Vaginal Birth After Cesarean (VBAC)
Today, it’s not unusual for a woman to have a vaginal delivery after a previous cesarean, called a VBAC. Be sure to discuss the pros and cons with your doctor.
Candidates for VBAC Births
According to the American College of Obstetricians and Gynecologists (ACOG), the following women could be candidates for a VBAC:
- The woman has had no more than one prior low-transverse cesarean delivery (This refers to the cut on your uterus, not the one on your belly)
- The woman has had no other uterine scars or ruptures, whether from previous cesareans or other surgeries
- The woman has a pelvis large enough to allow a vaginal delivery
- Delivery will be at an institution with a physician immediately available throughout active labor who can monitor the fetus and perform an emergent cesarean if needed
- Delivery at an institution where anesthesia and staff is immediately available if an emergency cesarean needs to be performed.
How to Request a VBAC
ACOG has specifically stated that whenever a woman is planning a VBAC delivery, there should be an appropriate medical team available, the resources to monitor a VBAC delivery and resources to provide an emergency cesarean if needed. Talk with your doctor about this option so they can help assemble the team needed to support your birth.

-
Immersion in warm water raises the body’s temperature and causes the blood vessels to dilate, resulting in increased circulation. The blood vessel dilation may help to lower the blood pressure of a laboring woman and decrease any fluid retention or swelling. Warm water also eases tension in the mother's shoulders and back, an important consideration for women experiencing back pain in labor.
Please note this option is not available at all of the Texas Health hospitals. Check with your healthcare provider if it may be an option available for you.
-
Natural Labor Support Techniques
A natural childbirth is one that looks for alternatives to the use of medical intervention. The goal is to increase a mother's confidence in her ability to give birth; classes help pregnant women understand how to cope with pain in ways that both facilitate labor and promote comfort, including focused breathing, movement and massage.
-
Labor Support Tools
Many of the Texas Health hospitals have birthing balls, labor bars, rocking chairs and some even have bathtubs or showers. Labor support tools may help you feel more comfortable and calm, ease the pain and stress of contractions, and promote the labor process. When you arrive at Labor and Delivery, please notify your nurse if you would like to use any of these items. Feel free to bring other labor-support tools.
-
Nitrous Oxide
Nitrous oxide can be administered during childbirth and is self-administered by a facial mask on the patient. Women who use it may still have an awareness of labor pain. Because it is self-administered, not only can a woman decide how much to use, but she can also decide if she wants to stop using it and try another method of pain relief instead. Nitrous oxide can be easily discontinued and its effects typically disappear quickly.
Please note this option is not available at all Texas Health hospitals. Check with your healthcare provider to learn whether it may be an option available.
-
Medications
There are a number of medications that may be delivered to you during labor via an IV.
A "systemic analgesic" is a pain-relieving medicine that is injected into your vein or muscle. This medicine acts on your entire nervous system rather than just a certain part of your body. The pain may be dulled but may not be eliminated completely.
-
Epidurals
An anesthesiologist or CRNA will inject a small bendable tube into the space in your lower back. This lessens the pain of the uterine contractions and the delivery of the baby through the vagina. Regional anesthetic (such as a spinal or an epidural) numbs the lower half of your body but leaves you awake and alert during the birth.
-
General Anesthesia
This medicine works on your whole body, and you will become unconscious and not feel any pain during the surgery. It may be used when a cesarean birth has to happen quickly. You will be given general anesthesia if you need a cesarean but cannot have an epidural or a spinal anesthesia.
An anesthesiologist or CRNA will give you the medicine in your IV. During the procedure, a tube is placed down your windpipe to help you breathe during the cesarean. After the baby is born, your provider closes the openings in your uterus and stomach. Then the medicine is stopped and you will wake up. Your throat may be sore for a few days because of the tube.
-
When You Arrive
Paperwork
Even if you preregistered, there will be some paperwork to fill out when you arrive. This paperwork gives us the authorizations to care for you and provides you with the opportunity to communicate your directive about the kind of care you want to receive, if desired. Your comfort is of the utmost importance to us so we will try to get you through this process as fast as possible.
Getting Checked In
After you’re checked in, typically you’ll be taken back to a triage area. Triage is a fancy word for where we will check you out initially and determine if you’re in active labor. A fetal monitor will be strapped to your belly to check the baby’s heart rate and measure your contractions. There will be a cervical check too, to see if you’ve dilated or effaced. If you are very far into labor, you will probably be immediately admitted and the triage experience will be bypassed.
If you are found to be in active labor, you will then be taken to a Labor and Delivery room. You will meet your Labor and Delivery nurse who will be your point person as you progress through labor.
-
Monitoring During Labor
In your Labor and Delivery room, the nurse will attach a fetal monitor to your stomach, either a wireless one or one connected to the bed. The fetal monitor will check your baby’s heart rate and monitor your contractions. During this time, we will have you reclining in bed. If everything is progressing well, intermittent monitoring may be possible and allow you to walk around to move things along.
Sometimes, an internal fetal monitor may be used to get a more accurate reading of heart rate and contractions. Know that every tool used in the delivery room is designed to help you safely meet your baby on delivery day.
-
Writing out a birth plan, going over it with your doctor or nurse-midwife ahead of time and sharing it with your Labor and Delivery nurse when you arrive, can help you achieve the birth experience you desire. Your birth plan may include information such as the type of delivery you desire and any plans for pain management. Remember things may not always go according to plan; our goal is to keep you and your baby safe. We encourage you to speak up if you’re concerned at any time about your care.
-
There will be lots of people in the room. Besides your nurse (probably more than one), the doctor and your significant other, there are a handful of other people that may be in the room, such as:
- Certified Nurse–Midwife — An independent healthcare provider who has received a bachelor’s degree in nursing and either a master’s or doctorate degree in midwifery.
- Doula — A person who can support you during your labor and act as an advocate for your care. These individuals are hired by the family to be present during the labor and birth.
- OB/GYN Hospitalist — An in-house, hospital-based doctor on the medical staff, who supports your physician by providing obstetric and gynecological care during emergencies and any time your own doctor is unavailable.
- Anesthesiologist and CRNA — Providers on the medical staff that determine the type and amount of anesthetic needed for patients. They also continually monitor patients' pulse, body temperature and other vital signs during surgery.
- NICU Team — A group of NICU nurses, respiratory therapists, neonatal nurse practitioners, etc. who are trained to care for infants born with special needs such as prematurity, low-birth weight or other medical issues.
- Surgical Scrub Technician — An individual who assists your physician in the operating room if you need to have a cesarean birth.
- Patient Care Technician — An individual who supports the patient during the labor and birth and can assist with various tasks, such as helping the patient to the restroom, changing bedding, etc.
-
What to Expect During Labor
Labor Can Take a Long Time
Every mom is different and first-time labors typically take the longest. To help cope with the waiting, make sure you have something to do. Bring a book to read, play a game on your phone, or watch on movie on your laptop. Surround yourself with family members and/or friends who will help you stay relaxed and focused.
Sadly, Vomit and Diarrhea Are Normal
Be prepared for some throwing up and/or diarrhea as your body gets ready for what’s ahead. The pain or pain medication may cause you to get sick. And as your uterus begins to contract (even if you can’t feel it yet), it irritates your bowel, which makes you have to go to the bathroom a lot.
Typically, No Eating During Labor
Typically, only clear liquids (water, apple juice, clear sodas, etc.) and ice chips may be allowed. If you can plan ahead, it may be good to grab a bite to eat before heading to the hospital, but make sure to double check with your provider.
-
When Can You Get an Epidural
Technically, you can get an epidural at any time during labor. Just know that it can slow down the labor process so it’s best to get it when you are further along. An epidural sends numbing medication to the area around your spinal cord via a catheter tube, and this makes you numb from the belly button down. Once you get the epidural, you might experience some shaking and chills because the epidural medicine is cold. You will receive continuous monitoring during this time, and you may also get an IV to provide fluids so you don’t get dehydrated and possibly a catheter to empty your bladder.
-
Pushing and Birth
As contractions become strong and close together, you might feel intense pressure, (sort of like having to go number two). Your doctor or nurse-midwife will tell you if it’s time to push, push hard or not so hard. It could take three pushes or 30.
Your doctor will also help guide your baby’s head out. You will continue to push to help deliver baby’s shoulders and body. After your baby is delivered, you will deliver the placenta, the organ that nourished your baby inside the womb.
You may poop when you push, and that’s totally ok! Because your contractions stimulate your bowels and you use the same muscles to poop as you do to push, it might happen.
-
After Your Birth
As soon as possible after birth, nurses will place your baby skin to skin until the first feeding is established. This procedure also helps the baby stay warm and stabilizes their blood-sugar level. After the first hour, your newborn will be examined and weighed. You and your baby will remain in Labor and Delivery for approximately two hours after the birth. Although at some hospitals, you will remain in the birth suite your entire stay.
One thing you may not realize, you may continue to have contractions, even after the baby is born.